Definition and Causes of Plantar Warts
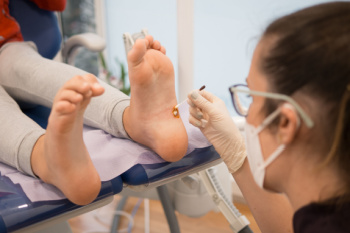
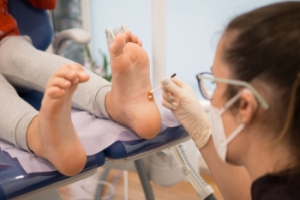
Plantar warts are small, rough growths that appear on the bottom of the feet, often on the heels or the balls of the feet. These warts are caused by the human papillomavirus, or HPV, which enters the skin through tiny cuts or breaks. The virus thrives in warm, moist environments, making public places like swimming pools or locker rooms common areas for infection. One of the most noticeable signs of plantar warts is the development of hard, thickened areas of skin, often with tiny black dots in the center, which are clogged blood vessels. The warts can cause discomfort, especially when pressure is applied, making walking or standing painful. In some cases, they may grow in clusters, which are called mosaic warts. If you have a plantar wart, it is suggested that you promptly schedule an appointment with a podiatrist who can offer effective treatment solutions, which may include removal for permanent relief.
Plantar warts can be very uncomfortable. If you need your feet checked, contact one of our podiatrists from Pennsylvania. Our doctors will assist you with all of your foot and ankle needs.
About Plantar Warts
Plantar warts are the result of HPV, or human papillomavirus, getting into open wounds on the feet. They are mostly found on the heels or balls of the feet.
While plantar warts are generally harmless, those experiencing excessive pain or those suffering from diabetes or a compromised immune system require immediate medical care. Plantar warts are easily diagnosed, usually through scraping off a bit of rough skin or by getting a biopsy.
Symptoms
- Lesions on the bottom of your feet, usually rough and grainy
- Hard or thick callused spots
- Wart seeds, which are small clotted blood vessels that look like little black spots
- Pain, discomfort, or tenderness of your feet when walking or standing
Treatment
- Freezing
- Electric tool removal
- Laser Treatment
- Topical Creams (prescription only)
- Over-the-counter medications
To help prevent developing plantar warts, avoid walking barefoot over abrasive surfaces that can cause cuts or wounds for HPV to get into. Avoiding direct contact with other warts, as well as not picking or rubbing existing warts, can help prevent the further spread of plantar warts. However, if you think you have developed plantar warts, speak to your podiatrist. He or she can diagnose the warts on your feet and recommend the appropriate treatment options.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
All About Plantar Warts
Plantar warts are warts that are only found on the feet, hence the term “plantar”, which means “relating to the foot.” They are caused by the human papillomavirus, or HPV, and occur when this virus gets into open wounds on the feet. The warts themselves are hard bumps on the foot. They are easily recognizable, mostly found on the heels or ball of the foot. Plantar warts are non-malignant, but they can cause some pain, discomfort, and are often unsightly. Removing them is a common step toward treating them.
Plantar warts can cause some pain while standing, sometimes felt as tenderness on the sole of your foot. Unless the wart has grown into the foot behind a callus, you will be able to see the fleshy wart. A podiatrist should only be consulted if there is an excessive amount of pain. Plantar warts are not cancerous or dangerous, but they can affect your walking and continually reappear. Anyone who suffers from diabetes or a compromised immune system disease should seek out care immediately.
Podiatrists are easily able to diagnose plantar warts. They usually scrape off a tiny bit of the rough skin to make tiny blood clots visible and examine the inside of warts. However, a biopsy can be done if the doctor is not able to diagnose them from simply looking at them. Although plantar warts usually do not require an excessive amount of treatment, there are ways to go about removing them. A common method is to freeze them off using liquid nitrogen, removing them using an electrical tool, or burning them off via laser treatment. For a less invasive treatment option, topical creams can be used through a doctor’s prescription. This treatment method takes more time, however. Keep the wart covered for protection in between daily treatments.
The best way to avoid developing plantar warts is to avoid walking barefoot in public places. Avoid this especially if you have open sores or cuts on your feet. It is also important to avoid direct contact with warts in general, as they are highly contagious.
Choosing Running Shoes for Different Distances

Selecting the right running shoes for various distances is vital to ensure comfort, prevent injury, and improve performance. For shorter distances, such as sprints or 5Ks, lightweight shoes with more flexibility are ideal. These shoes offer quick responsiveness, allowing for fast foot turnover. For longer distances, like half-marathons or marathons, shoes with more cushioning provide extra support and shock absorption to reduce the impact on joints. Support is also essential, particularly for runners who experience overpronation or underpronation. Stability shoes help correct these issues, offering a more controlled stride and reducing the risk of injury. Cushioning should be balanced with support, ensuring that the shoe does not feel too soft or too firm, which can lead to discomfort. Additionally, flexibility plays a role in ensuring natural movement, especially for long-distance runners, as it helps maintain proper form and minimizes fatigue. If you have endured a foot or ankle injury from wearing the wrong running shoes, it is suggested that you consult a podiatrist who can treat various foot conditions, and guide you on what type of shoes to wear.
You should always make sure your running shoes fit properly in order to avoid injury. For more information, contact one of our podiatrists from Pennsylvania. Our doctors can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
Improper shoe sizing can cause a myriad of problems for your feet. Shoes that don’t fit you properly can lead to muscular imbalances in your body, which can result in foot, knee, and hip injuries.
Tips for Finding the Right Running Shoe
- Make sure you have a thumb’s width of wiggle room between the end of your longest toe and the front of the shoe.
- There should be little to no slipping at the heel
- Don’t assume your size in one shoe brand will be your size in another
- Do not lace up your shoes too tightly
- Walk around in the store with your new shoes before you buy them
If you have any questions please feel free to contact our one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Choosing the Right Running Shoe
Choosing the right running shoes for you is an important part of running. A good pair of running shoes will make the running experience more enjoyable for you and prevent potential injury.
Poorly-fitted shoes can increase the risk of injury in runners substantially. Common injuries from running with poor quality shoes include shin splints, sprained ankles, Achilles tendinitis, stress fractures, plantar fasciitis and more. This is due to the fact that bad shoes do not provide proper foot support, can increase pronation (how much the foot rolls when hitting the ground), have little to no cushioning, do not allow the feet to breath, and do not provide enough flex and rigidity in the right parts.
When looking for running shoes, first, determine where you will be running. If you are a trail runner, then pick trail shoes. If you run on concrete and asphalt, then regular running shoes are the best choice. When trying on shoes, its best to go at the end of the day as feet grow during the day and shrink after a night of sleep. Shoes should be more rigid towards the back of the foot while being more flexible up where the toes are. The toe box should provide enough room for the toes to move freely. The overall fit should be snug, not too tight but not too loose. A good pair of running shoes should also provide enough arch support for your foot type. If you experience overpronation or under-pronation while running, try to find a pair of shoes that will help correct this with different sole patterns. Finally, try to find a pair of shoes that allow the feet to breathe like nylon mesh or synthetic leather.
Don’t forget about the socks either. Socks that hold too much moisture can lead to athlete’s foot. Socks should be breathable so that your feet can air out and breathe. Synthetic socks wick away moisture like sweat. If you tend to run a lot, having a second pair of shoes that you can wear while you let the first pair air out is smart. Just don’t forget to replace your shoes after about every 300 to 500 miles.
Before you start running, it is advised to see a podiatrist to see if running is right for you. They can also offer good advice on how to run and what to look for in a pair of running shoes. If you have flat feet or poorly supported ones, they can also offer custom-made orthotics that will help give your feet the support they need.
Grades and Risk Factors for Ankle Sprains

Ankle sprains occur when the ligaments surrounding the ankle are stretched or torn. They can range from mild to severe, depending on the extent of the damage. There are three main grades of ankle sprains. A Grade 1 sprain involves slight stretching of the ligaments, often causing mild pain and swelling. A Grade 2 sprain indicates a partial tear, resulting in moderate pain, swelling, and difficulty walking. A Grade 3 sprain is the most severe, where the ligament is completely torn, leading to significant pain, swelling, and instability. Several risk factors can increase the likelihood of an ankle sprain, including engaging in sports that involve jumping, running, or sudden changes in direction. Wearing improper footwear and having weak or imbalanced muscles are other risk factors. Symptoms of an ankle sprain typically include pain, swelling, bruising, and difficulty moving the ankle. If you have ankle pain and feel you may have sprained your ankle, it is suggested that you consult a podiatrist who can provide an accurate diagnosis and treatment.
Ankle sprains are common but need immediate attention. If you need your feet checked, contact one of our podiatrists from Pennsylvania. Our doctors can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains take place when the ligaments in your ankle are torn or stretched beyond their limits. There are multiple ways that the ankle can become injured, including twisting or rolling over onto your ankle, putting undue stress on it, or causing trauma to the ankle itself.
What Are the Symptoms?
- Mild to moderate bruising
- Limited mobility
- Swelling
- Discoloration of the skin (depending on severity)
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
Treatment of a sprain depends on the severity. Many times, people are told to rest and remain off their feet completely, while others are given an air cast. If the sprain is very severe, surgery may be required.
If you have suffered an ankle sprain previously, you may want to consider additional support such as a brace and regular exercises to strengthen the ankle.
If you have any questions please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ankle Sprains
Ankle sprains occur when ligaments that support the ankle stretch beyond their limits and tear. These types of injuries are very common and can occur in people of all ages. Sprains may range from mild to severe, depending on how much damage is done to the ligaments. If a sprain goes untreated, a more severe sprain may occur which can further damage the ankle. Repeated ankle sprains can lead to chronic ankle pain.
There are some risk factors that can increase your risk of suffering a sprained ankle. Those who participate in sports, walk on uneven surfaces, have a prior ankle injury, are in poor physical condition, or wear improper shoes are more likely to get a sprained ankle.
There are a few symptoms to look out for if you suspect you are suffering from a sprained ankle. Some common symptoms are swelling, bruising, tenderness, and instability of the ankle. In cases where the tearing of the ligaments is severe, there may be a “popping” sound when the strain occurs.
The RICE method is proven to be effective in treating ankle sprains. RICE stands for Rest, Ice, Compression, and Elevation. Rest is important for treatment, especially within the first 24 to 48 hours. You should also ice your sprained ankle for the first 48 hours for 20 minutes at a time. A small piece of cloth should be placed between the ice and the affected area. For the compression step, you should wear a brace that is snug, but not too tight that it cuts off circulation. When choosing a brace, be sure to choose one that is suitable for the type of ankle sprain you have. Lastly, you should elevate your foot above the heart as often as possible.
After you treat a sprain, you should go through rehabilitation to prevent the injury from occurring again. There are three phases to the rehab process. The first phase involves resting, protecting, and reducing the swelling of the injury. The second phase consists of restoring the ankle’s flexibility, range of motion, and strength. The third phase consists of slowly returning to activity and maintenance exercises.
If you suspect you have an ankle sprain, you shouldn’t hesitate to consult with your podiatrist. Your podiatrist will be able to give you a proper diagnosis and a suitable treatment option for your condition.
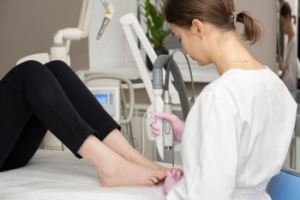
Laser Treatment for Toenail Fungus
Toenail fungus, also known as onychomycosis, causes nails to become thickened, discolored, and brittle. Laser treatment is a modern approach that uses concentrated light to target the fungus beneath the nail. The aim is to halt the growth of the fungus and promote healthier nails over time. This non-invasive treatment typically involves little to no discomfort, with most patients resuming normal activities immediately after a session. Results of laser toenail treatment may take several months to appear due to the slow regrowth of toenails. Multiple sessions may be necessary, as the effectiveness can vary based on the type of laser used and the severity of the infection. Laser toenail therapy also offers an alternative for people who cannot tolerate oral medications or who prefer to avoid their potential side effects. A podiatrist can evaluate the condition of your nails, recommend appropriate treatment options, and monitor your progress throughout the process. If you have developed a toenail fungus, it is suggested that you make an appointment with a podiatrist for an exam and to find out if laser toenail treatment is best for you.
If left untreated, toenail fungus may spread to other toenails, skin, or even fingernails. If you suspect you have toenail fungus it is important to seek treatment right away. For more information about treatment, contact one of our podiatrists of Pennsylvania. Our doctors can provide the care you need to keep you pain-free and on your feet.
Symptoms
- Warped or oddly shaped nails
- Yellowish nails
- Loose/separated nail
- Buildup of bits and pieces of nail fragments under the nail
- Brittle, broken, thickened nail
Treatment
If self-care strategies and over-the-counter medications does not help your fungus, your podiatrist may give you a prescription drug instead. Even if you find relief from your toenail fungus symptoms, you may experience a repeat infection in the future.
Prevention
In order to prevent getting toenail fungus in the future, you should always make sure to wash your feet with soap and water. After washing, it is important to dry your feet thoroughly especially in between the toes. When trimming your toenails, be sure to trim straight across instead of in a rounded shape. It is crucial not to cover up discolored nails with nail polish because that will prevent your nail from being able to “breathe”.
In some cases, surgical procedure may be needed to remove the toenail fungus. Consult with your podiatrist about the best treatment options for your case of toenail fungus.
If you have any questions, please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Treating Toenail Fungus
Fungal infection of the toenail, or onychomycosis, typically appears as a gradual change in a toenail’s texture and color that involves brittleness and darkening. The fungal infection itself occurs beneath the surface of the nail. Aside from discoloration, other symptoms include the collection of debris beneath the nail plate, white marks on the nail plate, and a foul odor emanating from the nail. If ignored, the infection can spread into other nails and the skin; in severe cases, it can hinder one’s ability to work or walk.
The toenails are particularly vulnerable to contracting infection in moist environments where people are likely to be walking barefoot, such as around swimming pools, public showers, and locker rooms. Fungal infection may also be more likely to occur in nail beds that have been injured, and sufferers of chronic diseases such as diabetes, circulatory problems, or immunodeficiency conditions are particularly prone to developing fungal nails.
Fungal nails can be primarily prevented by practicing proper hygiene and regularly examining the feet and toes. Carefully washing the feet with soap and water and thoroughly drying the feet afterwards are essential. Other tips include wearing shower shoes in public areas, changing shoes and socks daily, keeping toenails clipped at a short length, wearing breathable shoes that fit properly, wearing moisture-wicking socks, and disinfecting home pedicure tools and instruments used to cut nails.
Fungal nail treatment may vary between patients and the severity of the condition. Your podiatrist may suggest a daily routine of cleansing that spans over a period of time to ease mild infections. Over-the-counter or prescription antifungal agents may also be prescribed, including topical and/or oral medications. Debridement, or the removal of diseased nail matter and debris, may also be performed. In more severe cases, surgical treatment may be needed. In some instances, the temporary removal of the fungal nail allows for the direct application of a topical antifungal to the nail bed. In other cases, a chronically painful fungal nail that has not responded to other treatments may be permanently removed; this allows the infection to be cured and avoids the growth of a deformed nail.
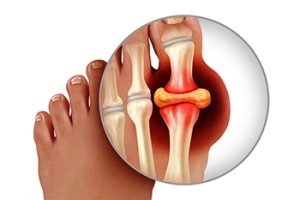
Why Gout Affects the Big Toe First
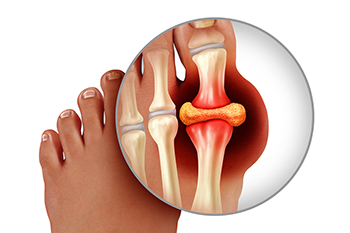
Gout is a form of arthritis caused by a buildup of uric acid crystals in the joints, leading to intense pain and inflammation. The big toe is often the first joint affected by gout due to its cooler temperature compared to other parts of the body. Uric acid tends to crystallize more easily in cooler areas, making the big toe, particularly the joint known as the first metatarsophalangeal joint, a prime target. Additionally, the big toe bears significant weight and stress while walking, which can further exacerbate the condition. When uric acid levels become elevated, the crystals accumulate in the joint, triggering inflammation and severe pain. Although gout can affect other joints over time, the big toe remains the most common initial site of attack. If you have gout, it is suggested that you are under the care of a podiatrist who can accurately diagnose and treat this painful condition.
Gout is a painful condition that can be treated. If you are seeking treatment, contact one of our podiatrists from Pennsylvania. Our doctors will treat your foot and ankle needs.
What Is Gout?
Gout is a form of arthritis that is characterized by sudden, severe attacks of pain, redness, and tenderness in the joints. The condition usually affects the joint at the base of the big toe. A gout attack can occur at any random time, such as the middle of the night while you are asleep.
Symptoms
- Intense Joint Pain - Usually around the large joint of your big toe, and it most severe within the first four to twelve hours
- Lingering Discomfort - Joint discomfort may last from a few days to a few weeks
- Inflammation and Redness -Affected joints may become swollen, tender, warm and red
- Limited Range of Motion - May experience a decrease in joint mobility
Risk Factors
- Genetics - If family members have gout, you’re more likely to have it
- Medications - Diuretic medications can raise uric acid levels
- Gender/Age - Gout is more common in men until the age of 60. It is believed that estrogen protects women until that point
- Diet - Eating red meat and shellfish increases your risk
- Alcohol - Having more than two alcoholic drinks per day increases your risk
- Obesity - Obese people are at a higher risk for gout
Prior to visiting your podiatrist to receive treatment for gout, there are a few things you should do beforehand. If you have gout you should write down your symptoms--including when they started and how often you experience them, important medical information you may have, and any questions you may have. Writing down these three things will help your podiatrist in assessing your specific situation so that he or she may provide the best route of treatment for you.
If you have any questions, please feel free to contact one of our offices located in Plymouth Meeting and Ambler, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.